Science behind hyperacusis diagnostic criteria
The criteria for diagnosis of hyperacusis based on the Hyperacusis Questionnaire (HQ; Khalfa et al. 2002) and Uncomfortable Loudness Levels (ULLs) are not generally agreed and there are wide differences in recommendations across studies (Aazh et al. 2018; Aazh et al. 2014; Blaesing & Kroener-Herwig 2012; Fackrell et al. 2015; Jastreboff & Jastreboff 2015; Meeus et al. 2010; Tyler et al. 2014). Moreover, there are conflicting reports with regard to the relationship between ULLs and patients’ self-reported hyperacusis handicap as measured via HQ (Aazh et al. 2017; Blaesing & Kroener-Herwig 2012; Meeus et al. 2010).
Most recent evidence-based cut-off scores for Hyperacusis Questionnaire (HQ) and Uncomfortable Loudness Levels (ULLs) indicating positive diagnosis for hyperacusis
Pioneering study by Dr. Aazh’s tinnitus team showed that a diagnosis of hyperacusis handicap based on HQ scores can be made consistent with a diagnosis based on ULLs if the following cut-off scores are adopted for a positive diagnosis: the average ULL at 0.25, 0.5, 1, 2, 4 and 8 kHz for the ear with the lower average ULL, ULLmin, should be ≤77 dB HL and the HQ score should be ≥22 (Aazh & Moore 2017). With these cut-off values, 95% of patients with HQ scores meeting the criterion will also meet the criterion based on ULLs, and vice versa.
The graphs show the distribution of different values of ULLmin and HQ scores among over 1000 patients who were seen by Dr. Aazh’s tinnitus team for tinnitus, and/or hyperacusis, and/or misophonia.
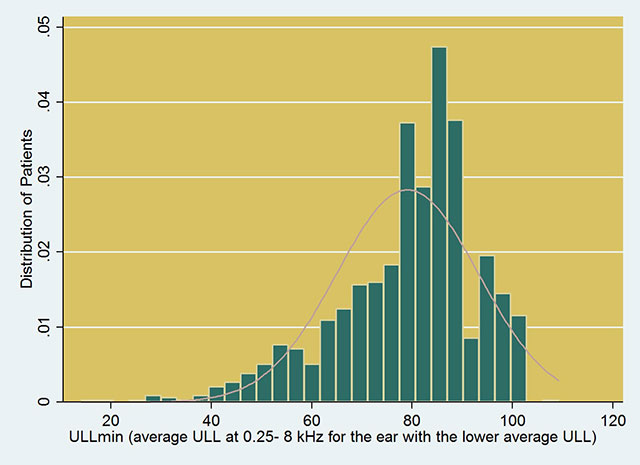
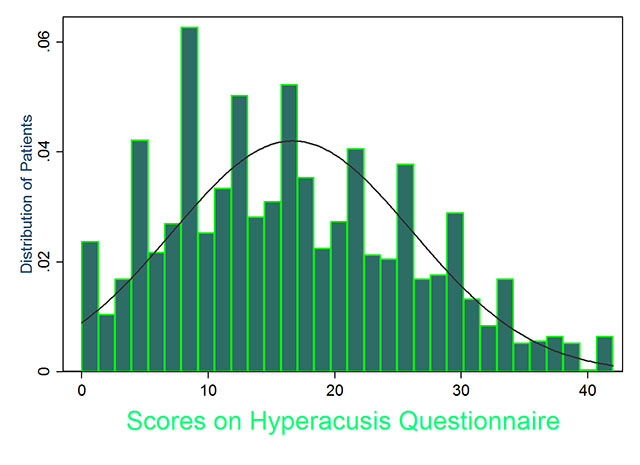
The analytical process that has led to the cut-off scores for HQ and ULLs
For patients with scores of 26 or above on the HQ as a cut-off which was suggested by Meeus et al. (2010), the mean value of ULLmin was 72.7 dB HL (SD =17 dB, n = 115, 95% confidence interval, CI= 69.6 to 75.8 dB HL). The mean was significantly (p < 0.001) lower than the mean value of ULLmin for patients with HQ scores below 26, which was 84.6 dB HL (SD = 13 dB, n = 359). See the histogram of ULLmin distribution for patients with HQ scores of 26 or above.
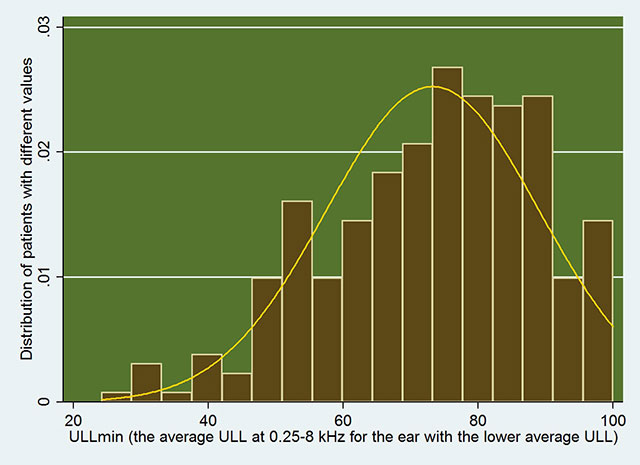
If the diagnosis of hyperacusis handicap were based on the value of ULLmin, a cut-off value of 76 dB HL (the upper limit of the 95% CI) would encompass 95% of those with significant hyperacusis handicap, as indicated by an HQ score of 26 or more. The mean HQ score was 16.3 (95% CI: 15.4 to 17.2) for patients with ULLmin >76 dB HL and was 23.6 (95% CI: 22 to 25.2) for patients with ULLmin ≤76 dB HL. This is both interesting and problematic, as it indicates that more than 95% of patients with ULLmin ≤76 dB HL have HQ scores below 26, i.e. not reaching the conventional HQ score used to diagnose hyperacusis handicap. See the histogram for HQ scores distribution among patients with ULLmin ≤76 dB HL.
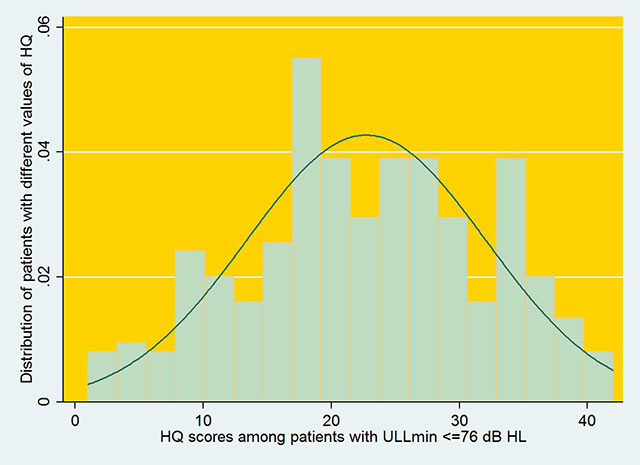
On these grounds, we believe that the threshold for diagnosing hyperacusis handicap using the HQ needs modification. If the score on the HQ indicating hyperacusis handicap is reduced to 22 (the lower end of the 95% CI for patients with ULLmin ≤76 dB HL), then repeating the above analysis leads to a better-matched outcome between reduced ULLs and abnormal scores on the HQ. For patients with HQ scores of 22 or above, the mean value of ULLmin was 74.4 dB HL (SD =17, n = 163) which was significantly (p < 0.001) lower than the mean value of ULLmin for patients with HQ scores below 22 (mean = 85.6 dB HL, SD = 12, n = 311). ). See the histogram of ULLmin distribution for patients with HQ scores of 22 or above.
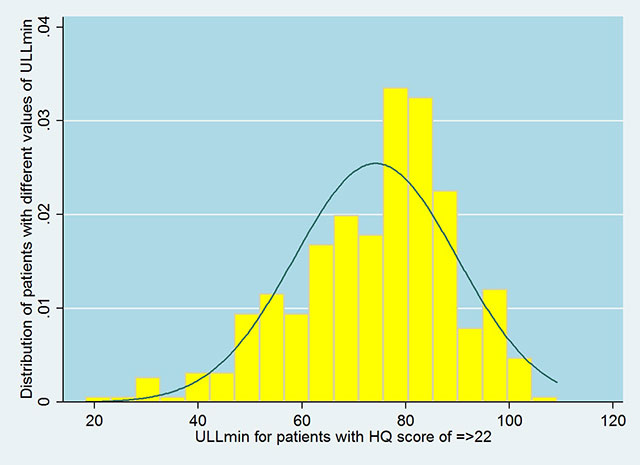
The boundaries of the 95% CI of the mean ULLmin for patients with HQ scores of 22 or above were 71.8 and 77 dB HL. Given the upper limit of 77 dB HL, it seems reasonable to propose that hyperacusis handicap is indicated by a ULLmin value of 77 dB HL or less. This ULL-based criterion would encompass 95% of those with significant hyperacusis handicap, as indicated by HQ scores of 22 or more. The mean HQ score was 16.1 (95% CI: 15.2 to 17) for patients with average ULLs for the worse ear above 77 dB HL and was 23.5 (95% CI: 22 to 25) for patients with average ULLs of the worse ear ≤77 dB HL. See the histogram of HQ distribution for patients with ULLmin of ≤77 dB HL.
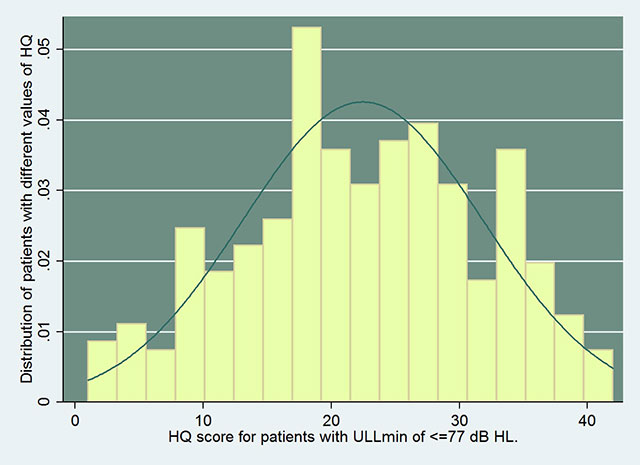
In summary, with appropriate choice of the cut-off values required for the diagnosis of hyperacusis handicap, a good correspondence can be obtained between diagnoses based on ULLs and on HQ scores. Appropriate cut-off values are ULLmin ≤77 dB HL and HQ score ≥22.
References
Aazh, H., Knipper, M., Danesh, A. A., et al. (2018). Insights from the third international conference on hyperacusis: causes, evaluation, diagnosis, and treatment. Noise Health, 20, 162-170.
Aazh, H., Lammaing, K., & Moore, B. C. J. (2017). Factors related to tinnitus and hyperacusis handicap in older people. International Journal of Audiology 56, 677-684.
Aazh, H., McFerran, D., Salvi, R., et al. (2014). Insights from the First International Conference on Hyperacusis: causes, evaluation, diagnosis and treatment. Noise Health, 16, 123-6.
Aazh, H., & Moore, B. C. J. (2017). Factors related to Uncomfortable Loudness Levels for patients seen in a tinnitus and hyperacusis clinic. International Journal of Audiology 56, 793-800.
Blaesing, L., & Kroener-Herwig, B. (2012). Self-reported and behavioral sound avoidance in tinnitus and hyperacusis subjects, and association with anxiety ratings. Int J Audiol, 51, 611-7.
Fackrell, K., Fearnley, C., Hoare, D. J., et al. (2015). Hyperacusis Questionnaire as a tool for measuring hypersensitivity to sound in a tinnitus research population. Biomed Res Int, 2015, 290425.
Jastreboff, P. J., & Jastreboff, M. M. (2015). Decreased sound tolerance: hyperacusis, misophonia, diplacousis, and polyacousis. Handb Clin Neurol, 129, 375-87.
Khalfa, S., Dubal, S., Veuillet, E., et al. (2002). Psychometric normalization of a hyperacusis questionnaire. ORL J Otorhinolaryngol Relat Spec, 64, 436-42.
Meeus, O. M., Spaepen, M., Ridder, D. D., et al. (2010). Correlation between hyperacusis measurements in daily ENT practice. Int J Audiol, 49, 7-13.
Tyler, R. S., Pienkowski, M., Rojas Roncancio, E., et al. (2014). A review of hyperacusis and future directions: part I. definitions and manifestations. American Journal of Audiology, 23, 402-419.
Read MoreCookie settings
REJECTACCEPT
Privacy Overview
| Cookie | Duration | Description |
|---|---|---|
| __stripe_mid | 1 year | Stripe sets this cookie cookie to process payments. |
| __stripe_sid | 30 minutes | Stripe sets this cookie cookie to process payments. |
| cookielawinfo-checkbox-advertisement | 1 year | Set by the GDPR Cookie Consent plugin, this cookie is used to record the user consent for the cookies in the "Advertisement" category . |
| cookielawinfo-checkbox-analytics | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Analytics". |
| cookielawinfo-checkbox-functional | 11 months | The cookie is set by GDPR cookie consent to record the user consent for the cookies in the category "Functional". |
| cookielawinfo-checkbox-necessary | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookies is used to store the user consent for the cookies in the category "Necessary". |
| cookielawinfo-checkbox-others | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Other. |
| cookielawinfo-checkbox-performance | 11 months | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Performance". |
| viewed_cookie_policy | 11 months | The cookie is set by the GDPR Cookie Consent plugin and is used to store whether or not user has consented to the use of cookies. It does not store any personal data. |
| Cookie | Duration | Description |
|---|---|---|
| _ga | 2 years | The _ga cookie, installed by Google Analytics, calculates visitor, session and campaign data and also keeps track of site usage for the site's analytics report. The cookie stores information anonymously and assigns a randomly generated number to recognize unique visitors. |
| _gat_gtag_UA_131443801_1 | 1 minute | Set by Google to distinguish users. |
| _gid | 1 day | Installed by Google Analytics, _gid cookie stores information on how visitors use a website, while also creating an analytics report of the website's performance. Some of the data that are collected include the number of visitors, their source, and the pages they visit anonymously. |
| CONSENT | 2 years | YouTube sets this cookie via embedded youtube-videos and registers anonymous statistical data. |
| Cookie | Duration | Description |
|---|---|---|
| VISITOR_INFO1_LIVE | 5 months 27 days | A cookie set by YouTube to measure bandwidth that determines whether the user gets the new or old player interface. |
| YSC | session | YSC cookie is set by Youtube and is used to track the views of embedded videos on Youtube pages. |
| yt-remote-connected-devices | never | YouTube sets this cookie to store the video preferences of the user using embedded YouTube video. |
| yt-remote-device-id | never | YouTube sets this cookie to store the video preferences of the user using embedded YouTube video. |
| yt.innertube::nextId | never | This cookie, set by YouTube, registers a unique ID to store data on what videos from YouTube the user has seen. |
| yt.innertube::requests | never | This cookie, set by YouTube, registers a unique ID to store data on what videos from YouTube the user has seen. |
| Cookie | Duration | Description |
|---|---|---|
| m | 2 years | No description available. |
